What is Postpartum Depression?
Postpartum depression (PPD) is a complex, multifaceted mental health condition that can affect new mothers, emerging typically within the first year after childbirth. Unlike the occasional mood swings and emotional fluctuations often referred to as the “baby blues,” which may resolve within a few days or weeks, postpartum depression is more severe and long-lasting. It can significantly impair a mother’s ability to care for herself and her newborn.
The prevalence of PPD varies, but studies suggest that approximately 10-20% of new mothers experience significant depressive symptoms following childbirth, indicating a substantial public health issue. Symptoms of PPD can manifest as persistent sadness, anxiety, irritability, difficulty concentrating, and feelings of worthlessness or guilt. These experiences can hinder a mother’s bonding with her child, impact family dynamics, and pose risks for both maternal and infant health.
Several factors contribute to the development of postpartum depression. Biologically, hormonal changes after childbirth can affect mood and emotional regulation. Psychologically, a history of mental health issues, lack of support, or stress related to new responsibilities can exacerbate feelings of depression. Social factors such as isolation, financial strain, and relationship challenges can also influence the likelihood of developing PPD.
Consequently, postpartum depression is not simply a consequence of hormonal imbalance; it results from the interaction of biological predispositions, psychological health, and social environment. Recognizing the seriousness of postpartum depression is paramount for both prevention and treatment. New mothers should not hesitate to seek help if they identify symptoms of PPD, as early intervention can facilitate recovery and foster better outcomes for both mother and child.
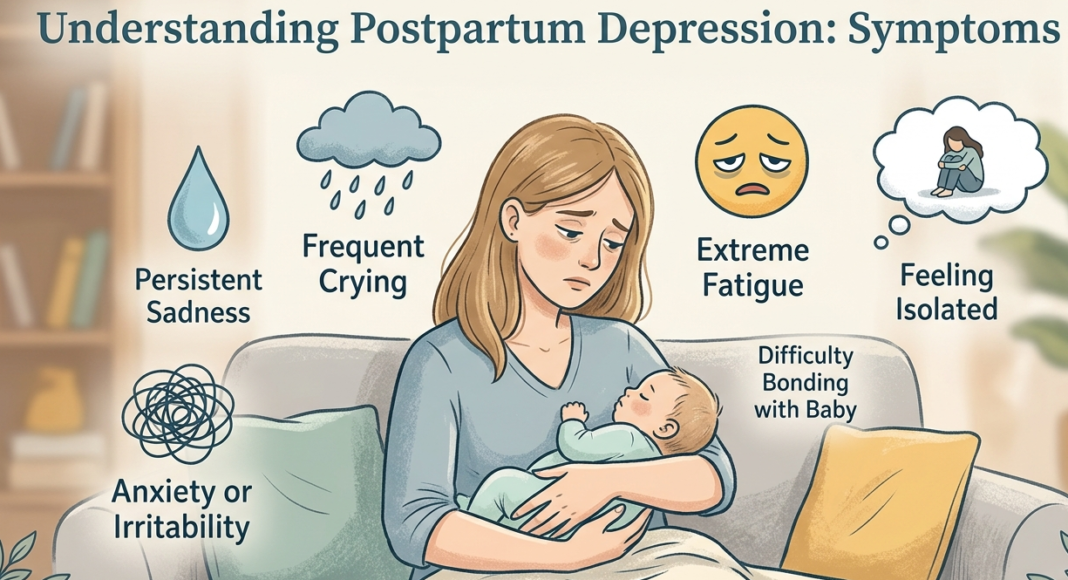
Common Symptoms of Postpartum Depression
Postpartum depression (PPD) encompasses a range of emotional and physical symptoms that can significantly affect new mothers. Understanding these symptoms is crucial for identifying PPD and seeking appropriate help. Emotionally, women may experience intense feelings of sadness, anxiety, or irritability that are more profound than the typical “baby blues”. A pervasive sense of inadequacy or guilt often accompanies these feelings, leading new mothers to question their ability to care for their newborn or to feel disconnected from their child.
Additionally, it is not uncommon for those experiencing postpartum depression to encounter a significant mood fluctuation. These emotional states can lead to a sense of hopelessness or despair, making daily tasks overwhelming. Anxiety may manifest in numerous ways, including persistent worry about the baby’s health, obsessing over minor details of parenting, or general panic about the future.
On the physical side, postpartum depression often presents itself through fatigue that extends beyond typical tiredness associated with caring for a newborn. This can be debilitating, impacting the mother’s ability to engage with her surroundings or to maintain the energy required for parenting duties. Changes in appetite are also prevalent; some new mothers may eat significantly less or turn to food as comfort, leading to weight fluctuations. Furthermore, sleep disturbances are common, with many affected by insomnia, despite the extreme fatigue, or oversleeping as an escape from their emotional turmoil.
The symptoms of postpartum depression can vary considerably in both intensity and duration. This variability can sometimes make it challenging for women to recognize that they may be struggling with a mental health condition. Therefore, understanding these symptoms is a vital first step towards effective management and recovery.
Risk Factors for Developing PPD
Understanding the risk factors associated with postpartum depression (PPD) can play a crucial role in early identification and intervention. Numerous factors can contribute to the likelihood of developing PPD, including personal and family histories, experiencing significant life stressors, and the availability of support systems.
Firstly, an individual’s personal history is significant. Those with a previous history of depression or anxiety disorders are at a higher risk of developing PPD after childbirth. Such conditions can predispose new mothers to hormonal changes and emotional challenges, heightening vulnerability in the postpartum period. Additionally, a family history of mental health issues also increases this risk. For instance, if a woman has close relatives who have suffered from mood disorders, she may have a genetic disposition that makes her more likely to experience PPD.
Stressful life events can further exacerbate the likelihood of PPD. Experiencing traumatic events, relationship issues, financial stress, or the loss of a loved one during or after pregnancy can significantly impact a new mother’s emotional well-being. These stressors can disrupt the delicate balance of hormones that occur after childbirth, triggering depressive symptoms.
The absence of a strong support system is another factor that can contribute to the development of postpartum depression. New mothers who feel isolated or lack emotional and practical support from partners, family, or friends may struggle to cope with the demands of motherhood, increasing the risk of mental health issues.
Additionally, other variables such as marital problems, socioeconomic challenges, and the experience of a difficult childbirth can all further influence mental health outcomes postpartum. Recognizing these risk factors can empower expecting mothers and their families to seek appropriate support and interventions that may mitigate the effects of postpartum depression.
How Postpartum Depression Differs from Other Conditions
Postpartum depression (PPD) is a complex condition that often presents itself after childbirth, and while some symptoms may overlap with other disorders, it is essential to distinguish PPD from related conditions such as postpartum anxiety, postpartum psychosis, and the baby blues. Recognizing these differences can be crucial for effective treatment and management.
Postpartum anxiety, for instance, manifests primarily through excessive worry, irritability, and physical symptoms like racing heart and shortness of breath. Unlike PPD, which predominantly involves persistent feelings of sadness and hopelessness coupled with a loss of interest in life, postpartum anxiety focuses more on heightened fears regarding the baby’s health and well-being. Furthermore, while anxiety may coexist with depression, women suffering from postpartum depression experience a more profound sense of emotional devastation that hinders their ability to perform daily activities.
On the other hand, postpartum psychosis is a rare but severe condition that typically occurs within the first two weeks after childbirth. It is marked by disturbing thoughts, hallucinations, or delusions, which can pose a serious risk to both the mother and the infant. This condition requires immediate psychiatric intervention. In contrast, the symptoms of postpartum depression are usually less acute and develop gradually over weeks or months. They can range from mild to severe and require various levels of support.
Lastly, the baby blues are a transient and common condition experienced by many new mothers, characterized by mood swings, crying spells, and feelings of being overwhelmed. While the baby blues generally fade within two weeks, postpartum depression persists longer and may require professional help. Understanding these distinctions is vital for new mothers and their families to ensure adequate care and support is provided.
Impact of Postpartum Depression on Mothers and Families
Postpartum depression (PPD) is a pervasive mental health condition that significantly affects not just the new mother but also extends its impact to her partner and the entire family unit. The emotional and psychological toll of PPD can disrupt the delicate dynamics of familial relationships and bonding experiences, crucial in the early stages of a child’s life.
For mothers experiencing postpartum depression, feelings of isolation, anxiety, and sadness are common. These emotional struggles can seriously hinder the ability to connect with their newborn, leading to problematic attachment and bonding, which are essential for the child’s emotional and cognitive development. According to various studies, mothers with PPD may find themselves less responsive to their infants’ needs, which can affect the child’s overall emotional well-being.
Furthermore, the consequences of PPD can ripple through family dynamics. Partners may struggle to support the mother, feeling helpless or frustrated as they witness her distress. This scenario often leads to increased tension and conflict within the relationship. As the partner attempts to navigate their partner’s condition and the challenges of parenthood, they may also experience feelings of anxiety or depression, creating a cycle of emotional strain that detracts from the family’s well-being.
Additionally, siblings of the newborn may sense the emotional unrest in the household, potentially leading to behavioral issues or feelings of neglect. Family members may be forced to adjust their roles and responsibilities, which can create further disruptions in routine and stability. As a result, the overall caregiver well-being is compromised, making it crucial to identify and address postpartum depression as early as possible.
When to Seek Help: Signs and Situations
Recognizing the appropriate time to seek help for postpartum depression (PPD) is crucial for the well-being of the mother and her family. There are specific situations and signs that indicate professional intervention is necessary. Initially, it is important to acknowledge that while experiencing mild symptoms can be a part of the postpartum adjustment, severe symptoms that persist beyond a few weeks should not be overlooked.
One of the prominent signs that indicate the need for immediate help includes the experience of intense feelings of sadness or anxiety. If these feelings disrupt daily activities and hinder the ability to care for oneself or the newborn, it is vital to seek help. Moreover, women who experience any form of emotional numbness or detachment from their baby, coupled with feelings of guilt or worthlessness, should promptly consult a healthcare professional.
Another critical time to seek help is during any crises or moments when thoughts of self-harm or harming the baby arise. Such thoughts can be an indication of a more severe form of PPD and require immediate attention from a mental health professional. Additionally, if symptoms related to the postpartum condition worsen or symptoms begin to manifest in new forms, swift action is warranted.
Finally, it is essential to recognize that the experience of postpartum depression can vary significantly among individuals. Therefore, if a mother feels that traditional coping mechanisms or support systems are falling short, it is crucial to reach out for professional guidance. The earlier professional help is sought, the better the chances for recovery and well-being for both the mother and child.
Treatment Options for Postpartum Depression
Treatment for postpartum depression (PPD) can be approached through various pathways, tailored specifically to each individual’s needs. An effective treatment plan typically combines therapeutic interventions, medication, and lifestyle adjustments. Among the most commonly used psychotherapeutic approaches are cognitive-behavioral therapy (CBT) and interpersonal therapy (IPT). CBT focuses on identifying and altering negative thought patterns associated with depression, thereby fostering healthier perspectives about oneself and one’s situation. IPT, on the other hand, concentrates on improving personal relationships and enhancing social supports, which can be crucial for new mothers experiencing PPD.
In addition to therapy, medication may also be a vital part of treatment for postpartum depression. Antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), are often prescribed to help alleviate symptoms. These medications can be effective in restoring the balance of neurotransmitters in the brain, thus improving mood and reducing feelings of anxiety. It is essential to discuss any potential risks and benefits of medication with a qualified healthcare provider, especially for those who are breastfeeding.
Besides therapy and medication, certain lifestyle changes can significantly bolster recovery from postpartum depression. Regular physical activity, for instance, can lead to enhanced physical wellness and improve mood through the release of endorphins, known as “feel-good” hormones. A balanced diet rich in essential nutrients also plays a critical role in mental health. Furthermore, prioritizing sleep and establishing a strong support network can aid new mothers in coping with the demands of parenthood while managing their mental well-being.
Ultimately, a personalized treatment plan that incorporates therapy, medication, and lifestyle changes ensures that the unique circumstances surrounding each case of postpartum depression are addressed effectively. Engaging with healthcare professionals who understand the complexities of PPD is crucial in guiding individuals toward the most suitable treatment options.
Support Systems: Finding Help
Building a strong support system is crucial for new mothers experiencing postpartum depression (PPD). A solid network not only provides emotional support but also serves as a resource for practical help. Support can come from various sources, including family and friends, healthcare providers, support groups, and community organizations.
Family and friends play an essential role in a new mother’s recovery. Open communication about feelings and experiences can foster empathy and understanding. Loved ones can also assist with daily tasks like childcare, household chores, or simply providing companionship, which can alleviate feelings of isolation that often accompany PPD.
Healthcare providers are another vital component in building a support system. Obstetricians, pediatricians, and mental health professionals can offer guidance and treatment options tailored to individual needs. Regular check-ups and consultations can help monitor the severity of symptoms and facilitate interventions if necessary. It is essential for mothers to feel comfortable discussing their mental health with their doctors to receive appropriate care.
Support groups specifically designed for mothers dealing with postpartum depression are excellent resources. These groups provide a safe environment to share experiences, gain insights, and receive encouragement from those who understand the challenges of motherhood and mental health. Many local hospitals, community centers, and online platforms offer such supports. Connecting with individuals who have experienced similar struggles can be incredibly therapeutic.
In addition to personal and professional support, various community resources can further assist new mothers. Programs may include access to parenting classes, workshops on mental health awareness, and local agencies that provide family support services. Exploring these resources can empower mothers by enhancing their coping strategies while fostering a sense of community. Finding and utilizing these support systems significantly alleviates the burden of postpartum depression and promotes recovery.
Conclusion and Encouragement
Postpartum depression (PPD) is a significant mental health condition that can affect new mothers, yet it remains widely misunderstood. Throughout this blog, we have highlighted the symptoms of PPD, which can range from feelings of extreme sadness and anxiety to sleep disturbances and difficulty bonding with the baby. Recognizing these symptoms is crucial, as it can lead to timely intervention and support. Women need to understand that experiencing postpartum depression is not a personal failure but a complex response to childbirth and the associated changes in life.
Seeking help is essential, and it is important to know that various resources are available. Reach out to healthcare professionals, who can provide the necessary evaluations and treatment options. Support groups can also be an invaluable resource, allowing mothers to share their experiences and feelings with others who can genuinely empathize.
It is important not only to acknowledge and discuss the challenges associated with postpartum depression but also to focus on the hope and recovery that is attainable. Many women have successfully navigated this journey and emerged stronger. By taking proactive steps, such as engaging in therapy, joining support networks, and talking openly about their feelings, new mothers can find effective coping strategies to combat the feelings of isolation and despair that often accompany PPD.
In essence, those who are experiencing postpartum depression should understand that they are not alone. It is perfectly acceptable to ask for help and to prioritize mental health. Healing is possible, and encouragement from family, friends, and mental health professionals can be instrumental in the road to recovery. By acknowledging one’s feelings and seeking support, it is possible to embrace the joys of motherhood while overcoming the challenges of postpartum depression.